Should You Be Afraid Of Having Root Canal Treatment?
Canterbury dentist, Dr George Mathioudakis, explains this sometimes feared treatment.
It is probably fair to say that few people look forward to a dental visit. Even if you are fairly sure that your teeth are in good condition, there is always the possibility that the dentist will find some decay or a crack that requires treatment.
While all but the most anxious patients will tend to shrug and accept the need for minor restorations like fillings, the same often cannot be said when they are told that they need to have a root canal procedure. However, as we’ll see below, their fears are usually unfounded, which hopefully comes as good news!
More than any other dental treatment, this is the one that most patients seem to fear. No one seems entirely sure about why this is the case, but perhaps the most plausible theory is that, before the regular use of x-rays, it would not have been possible to have detected any abscesses that were present before the treatment started. If contact was made with one of these during the treatment, it would have been excruciating for sure. Patients will be happy to hear though, that x-rays are now always routinely taken, and, if an abscess is found, it will be treated before the treatment takes place.
Why do you need root canal treatment?
At Bradley and Partners Dental and Implant Clinic, we believe in retaining the natural tooth wherever this is possible, extracting it only when necessary, or where a very poor prognosis warrants it. In many cases, restoration is achieved by using a filling or a crown. Where decay is very extensive though, this can reach the inner part of the tooth, in the root canals, where the nerves and tiny blood vessels are stored.
Once this part of the tooth is infected, the part we sometimes refer to as the ‘pulp’, it cannot be treated with antibiotics or other non invasive methods, and, to retain the tooth, the infected material needs to be removed, and the tooth restored.
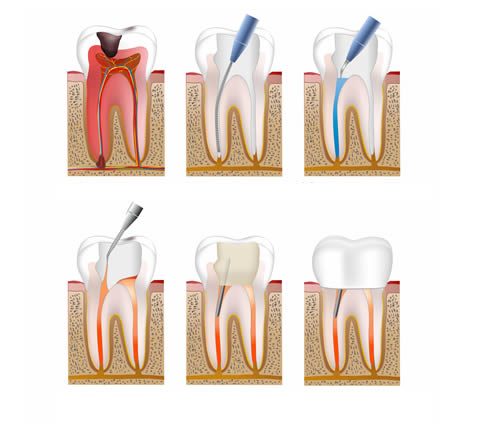
Root canal procedure – part one
The first part of the procedure is the preparation. This involves not only examining the tooth, but taking x-rays too. This enables us to see what is going on deep down in the tooth, as well as discovering if you have an abscess or not. Providing that you don’t, the actual treatment can go ahead.
The first part of this involves first of all, numbing the area with a local anaesthetic. Once this has taken effect, the dentist will remove part of the top section of the tooth. This enables the dentist to commence the ‘cleaning’ of the root canals.
Root canal procedure – part two
Once the infected pulp has been accessed, the next task is to remove this completely. This is done with a combination of suction equipment and manual removal. It is vitally important that all of the infected material is removed otherwise reinfection could occur. To make sure of this, the hollow canals will be thoroughly cleaned once the bulk of the pulp has been removed. Once this is done, the remaining part of your tooth will be infection free, but in a weakened state.
Root canal procedure – part three
The next step in this procedure is to fill in the now hollow canals. This is done using a special filling material that is largely only used for this procedure. This material, called gutta percha, is excellent for this purpose as it seals the canals completely, meaning that reinfection is very unlikely. Its bio-compatibility and sealant qualities make it an ideal material for this purpose.
Root canal procedure – part four
Your tooth is now infection free and the canals have been sealed, preventing re-infection. Leaving the tooth in this condition though means that it probably would not last very long due to its weakened state.
To both strengthen the treated tooth and to restore it to a relatively natural appearance, a dental crown will be used to ‘cap’ the tooth. By doing so, your tooth will not only feel natural, but you will be able to use it as you would a healthy tooth, with just a few caveats (see next section).
The end result
With a root canal treated tooth, all of the nerves have been removed and you will find that it feels ‘dead’, with no sensations. This means that you will not be able to feel any pain if the tooth starts to decay. It also means that you will need to be a little careful when eating as it is difficult to know how much pressure you are applying to it. A tooth that has undergone this procedure is also likely to be less strong than a healthy tooth. So with this in mind, you should take a little extra care.
Try not to use that tooth for eating harder foods as too much force could cause it to fracture. Try to use the other side of your mouth for this purpose, or generally avoid harder foods. For most purposes though, you will be able to eat normally.
You should also take care to clean the tooth and surrounding gum tissue. Although you may not have a toothache if decay occurs, any decay or breakage of the tooth may mean that the crown no longer fits securely, and could even become detached. Gum disease is also a possibility, so make sure to maintain a good cleaning regime at home, along with having a six monthly check up with one of our Canterbury dentists, or more frequently if requested.
We understand that patients can feel a little afraid about some procedure, and, to that end, we are always happy to explain a procedure in straightforward terms as best as we can. All patients, whether nervous or not, can be sure that they will be in safe and experienced hands when attending Bradley and Partners Dental and Implant Clinic.
If you would like to discuss any dental matter with us, or to make an appointment, please call our Canterbury clinic on 01227 463529.
